-
20/04
Thứ 7 -
21/04
CN -
22/04
Thứ 2 -
23/04
Thứ 3 -
24/04
Thứ 4 -
25/04
Thứ 5 -
26/04
Thứ 6
 VĐQG Ý
VĐQG Ý

 Lazio Roma
Lazio Roma
 Juventus Turin
Juventus Turin VĐQG Ả Rập Xê Út
VĐQG Ả Rập Xê Út

 AL Hilal Riyadh
AL Hilal Riyadh
 Damac FC
Damac FC VĐQG Đức
VĐQG Đức

 Augsburg
Augsburg
 Bochum
Bochum
 Darmstadt
Darmstadt
 M´Gladbach
M´Gladbach
 RB Leipzig
RB Leipzig VĐQG Tây Ban Nha
VĐQG Tây Ban Nha

 Granada CF
Granada CF
 Las Palmas
Las Palmas
 Osasuna
Osasuna VĐQG Pháp
VĐQG Pháp

 FC Lorient
FC Lorient
 Stade Rennes
Stade Rennes Ngoại Hạng Anh
Ngoại Hạng Anh

 Chelsea
Chelsea
 Brentford
Brentford
 Newcastle
Newcastle
 Burnley
Burnley
 Man City
Man City VĐQG Ý
VĐQG Ý

 SSC Napoli
SSC Napoli
 Udinese Calcio
Udinese Calcio
 US Lecce
US Lecce
 Frosinone Calcio
Frosinone Calcio FA Cúp Anh
FA Cúp Anh

 Chelsea
Chelsea
 Man United
Man United VĐQG Tây Ban Nha
VĐQG Tây Ban Nha

 Real Betis
Real Betis
 Cadiz
Cadiz
 Real Sociedad
Real Sociedad
 Villarreal
Villarreal VĐQG Đức
VĐQG Đức

 Bayern Munich
Bayern Munich
 Stuttgart
Stuttgart
 Leverkusen
Leverkusen VĐQG Ả Rập Xê Út
VĐQG Ả Rập Xê Út

 AL Ittihad
AL Ittihad
 AL Wehda (KSA)
AL Wehda (KSA) Ngoại Hạng Anh
Ngoại Hạng Anh

 Arsenal
Arsenal
 Nottingham Forest
Nottingham Forest
 AFC Bournemouth
AFC Bournemouth
 West Ham
West Ham
 Liverpool
Liverpool VĐQG Pháp
VĐQG Pháp

 Clermont Foot
Clermont Foot
 Racing Strasbourg
Racing Strasbourg
 Montpellier HSC
Montpellier HSC
 Metz
Metz
 AS Monaco
AS Monaco MLS Mỹ
MLS Mỹ

 Portland Timbers
Portland Timbers
 FC Cincinnati
FC Cincinnati
 Nashville SC
Nashville SC
 Orlando City SC
Orlando City SC
 DC United
DC United
 New England Revolution
New England Revolution
 Real Salt Lake
Real Salt Lake
 Austin FC
Austin FC
 Saint Louis City SC
Saint Louis City SC
 FC Dallas
FC Dallas
 NY Red Bulls
NY Red Bulls
 Vancouver
Vancouver Giao Hữu Quốc Tế
Giao Hữu Quốc Tế

 Estonia U17 (W)
Estonia U17 (W)

 VĐQG Ý
VĐQG Ý

 ACF Fiorentina
ACF Fiorentina
 Atalanta Bergamasca
Atalanta Bergamasca VĐQG Tây Ban Nha
VĐQG Tây Ban Nha

 Atletico Madrid
Atletico Madrid
 FC Barcelona
FC Barcelona VĐQG Pháp
VĐQG Pháp

 Olympique Marseille
Olympique Marseille
 Olympique Lyon
Olympique Lyon VĐQG Đức
VĐQG Đức

 Mainz
Mainz MLS Mỹ
MLS Mỹ

 Minnesota United FC
Minnesota United FC
 San Jose Earthquakes
San Jose Earthquakes Giao Hữu Quốc Tế
Giao Hữu Quốc Tế

 Morocco U18
Morocco U18
 Ecuador U18
Ecuador U18 VĐQG Ý
VĐQG Ý

 Bologna FC
Bologna FC
 Inter Milan
Inter Milan VĐQG Tây Ban Nha
VĐQG Tây Ban Nha

 Mallorca
Mallorca AFC Cup
AFC Cup

 AL Ahed
AL Ahed
 FC Abdysh-Ata Kant
FC Abdysh-Ata Kant Giao Hữu Quốc Tế
Giao Hữu Quốc Tế

 Switzerland U18
Switzerland U18
 GuatemalaU18
GuatemalaU18
 Belgium U16 (W)
Belgium U16 (W)
 Slovakia U18
Slovakia U18 AFC Champions
AFC Champions

 AL Ain FC
AL Ain FC
 Ulsan Hyundai
Ulsan Hyundai Ngoại Hạng Anh
Ngoại Hạng Anh

 Chelsea
Chelsea VĐQG Pháp
VĐQG Pháp

 Paris Saint-Germain
Paris Saint-Germain
 Lille OSC
Lille OSC
 OGC Nice
OGC Nice Ngoại Hạng Anh
Ngoại Hạng Anh

 AFC Bournemouth
AFC Bournemouth
 Newcastle
Newcastle
 Sheffield United
Sheffield United
 Liverpool
Liverpool VĐQG Ả Rập Xê Út
VĐQG Ả Rập Xê Út

 Al Tai
Al TaiĐôi nét về trang cập nhật thông tin Bongdaplus
Tên đầy đủ của trang web bóng đá này là “Tạp chí điện tử bóng đá,” là một trong ba trang tin thuộc cơ quan truyền thông đại diện cho Liên đoàn Bóng đá Việt Nam. Được cấp phép hoạt động chính thức vào cuối năm 2010, trang web này nhanh chóng đạt được vị trí hàng đầu trong danh sách các trang web bóng đá trực tuyến tại Việt Nam.
Dữ liệu mà kênh Bongdalu cung cấp cho người dùng không chỉ đa dạng mà còn chất lượng đỉnh cao. Người dùng có thể dễ dàng tìm kiếm mọi thông tin, đáp ứng nhanh chóng và đảm bảo tính xác thực. Việc truy cập vào kênh mỗi ngày không chỉ là lựa chọn thông minh, mà còn là bước tiến quan trọng, đặc biệt trong bối cảnh xuất hiện nhiều kênh bóng đá chất lượng kém.
Thông tin Bóng đá
Khi truy cập trang chủ của bongdalu vip, người dùng ngay lập tức tiếp cận với một loạt tin tức bóng đá mới nhất trong ngày. Các nội dung như tin chuyển nhượng, thông tin nóng về cầu thủ, và các thông báo từ các liên đoàn bóng đá danh tiếng sẽ được cập nhật nhanh chóng. Mọi thông tin có sức ảnh hưởng đều được hiển thị trên trang chủ.
Mục tin tức giúp người đọc nắm bắt tình hình bóng đá toàn cầu. Tin tức được thu thập từ các nguồn tin uy tín trên thế giới hoặc do các phóng viên chuyên nghiệp đưa tin. Sau khi biên tập, tin tức sẽ được đặt thành các tiêu đề hấp dẫn để thu hút độc giả.
Các tin tức nổi bật sẽ xuất hiện đầu trang của Bongdaplus, thậm chí có hình ảnh minh hoạ giúp người đọc hình dung sự kiện. Tiêu đề ngắn gọn nhưng hấp dẫn để người đọc có thể hiểu được nội dung.
Lịch Thi Đấu
Cập nhật lịch thi đấu hàng ngày giúp người dùng tổ chức thời gian để theo dõi trực tiếp các trận đấu bóng đá. Đồng thời, người dùng không bỏ lỡ những trận đấu hấp dẫn nhất. Bongdaplus cam kết cung cấp lịch thi đấu nhanh và chính xác, ngay sau khi thông tin chính thức được công bố. Lịch thi đấu sẽ cung cấp thông tin quan trọng như đội bóng thi đấu (đội chủ nhà được đặt trước), giờ và ngày thi đấu. Các trận đấu sẽ được sắp xếp theo từng giải đấu để người hâm mộ dễ dàng theo dõi.
Bảng xếp hạng
Ngoài việc theo dõi lịch thi đấu, người hâm mộ cũng cần liên tục cập nhật bảng xếp hạng bóng đá để nắm bắt vị trí hiện tại của các đội bóng trong các giải đấu. Trang web bongdalu vip là nguồn thông tin đáng tin cậy, cung cấp bảng xếp hạng của các giải đấu bóng đá nổi tiếng, thu hút sự quan tâm của cộng đồng người hâm mộ Việt Nam.
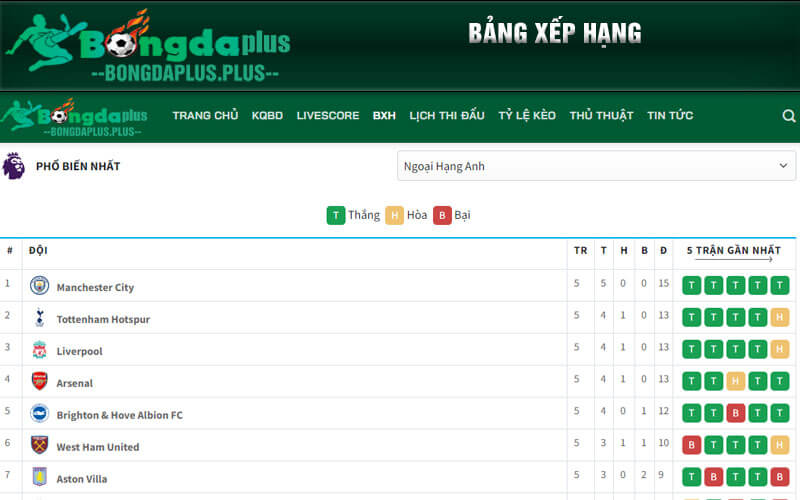
Bảng xếp hạng của Bongdaplus sẽ chứa đựng các thông tin chi tiết sau đây: Tổng số trận đã thi đấu trong mùa giải, số trận thắng – hòa – bại, hiệu số bàn thắng – thua, tổng số điểm, và kết quả của 5 trận đấu gần đây nhất. Đặc biệt, không thể bỏ qua thứ hạng hiện tại của từng đội. Qua bảng xếp hạng, người hâm mộ sẽ có cái nhìn tổng quan về đội nào đang nắm giữ cơ hội vô địch và đội nào đang đối mặt với nguy cơ xuống hạng trong mùa giải kế tiếp.
Kết quả bóng đá
Website Bongdaplus sẽ liên tục cập nhật kết quả bóng đá ngay sau mỗi trận đấu và tổng kết sau khi trận đấu kết thúc. Ngoài thông tin về tỷ số trực tuyến, người dùng còn có thể tìm thấy các dữ liệu quan trọng như tên các cầu thủ ghi bàn, thời điểm ghi bàn, và thông tin về các cầu thủ nhận thẻ phạt. Nhờ vào những thông tin này, người hâm mộ có thể nắm bắt kết quả trận đấu mà không cần phải xem trực tiếp.
Kết quả bóng đá plus sẽ được cập nhật ngay lập tức nhờ vào công nghệ livescore phổ biến hiện nay. Mọi khi có bàn thắng được ghi nhận trên sân, hệ thống livescore của Bongdaplus sẽ ngay lập tức cập nhật thông tin. Độ chính xác của việc cập nhật dữ liệu được đảm bảo là tuyệt đối.
Nhận định bóng đá
Nhận định bóng đá là một phần quan trọng không thể thiếu trên trang web Bongdaplus, và chúng tôi cam kết đặc biệt đến việc cung cấp thông tin đầy đủ và chính xác. Mỗi ngày, chúng tôi liên tục cập nhật hàng chục bài viết nhận định về những trận đấu nóng hổi nhất. Nhờ những bài viết này, bạn có thể nắm bắt được đội bóng nào đang được đánh giá cao và có tỷ số dự đoán cụ thể cho từng trận đấu.
Đội ngũ chuyên gia của chúng tôi dựa vào phong độ gần đây của các đội bóng, cùng với lịch sử đối đầu trong quá khứ để đưa ra nhận định chi tiết về mỗi trận đấu. Họ từ đó xây dựng tỷ số dự đoán chung cuộc với mức độ chính xác cao nhất có thể. Tuy nhiên, quan trọng nhất là bạn không chỉ nên xem tỷ số dự đoán, mà còn nên đọc cả bài viết để hiểu rõ hơn về lý do mà chuyên gia đã có những dự đoán nhất định. Điều này giúp bạn hiểu rõ hơn về cơ sở lý luận và thông tin mà họ đặt nền móng cho quan điểm của mình.
Soi kèo bóng đá
Chắc chắn rằng cộng đồng người hâm mộ bóng đá đang rất háo hức chờ đợi thông tin cá độ, và chuyên mục này là nguồn tin không thể bỏ qua. Được xây dựng bởi đội ngũ chuyên gia tài năng từ bdplus, chuyên mục soi kèo bóng đá hàng ngày đăng tải hàng trăm bài viết liên quan đến các trận đấu sắp diễn ra. Thông thường, những bài viết này sẽ xuất hiện trên Bongdaplus khoảng 10 giờ trước giờ bóng lăn, nhằm đảm bảo tính chính xác tối đa.
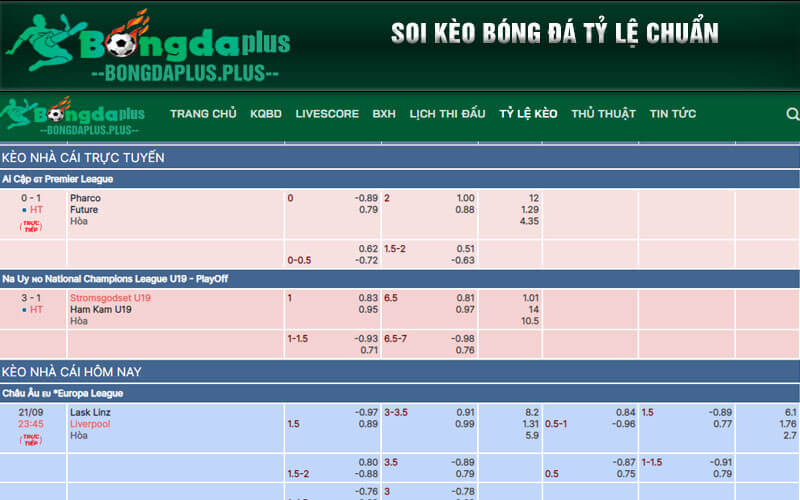
Các chuyên mục phổ biến nhất được thảo luận trong các bài viết soi kèo chủ yếu tập trung vào các loại kèo như kèo châu Á, kèo châu Âu, kèo xiên, và kèo tài xỉu. Từ đánh giá về khả năng thi đấu của các đội bóng, chuyên gia của Bongdaplus thường xuyên phân tích và đưa ra dự đoán về việc người chơi nên đặt cược vào lựa chọn nào, dựa trên tỷ lệ kèo từ các nhà cái. Với sự hỗ trợ của chứng cứ đầy đủ và lý luận sắc bén, người dùng có thể tin tưởng hoàn toàn vào chuyên mục soi kèo bóng đá này.
Bên cạnh các chuyên mục cơ bản, trang web Bongdaplus còn cung cấp nhiều chủ đề khác nhau, mang đến những nội dung thú vị mà không phải trang web bóng đá nào cũng có. Cụ thể:
- Lăng kính: Xuất bản các bài viết thể hiện quan điểm cá nhân của tác giả thông qua lời văn hóm hỉnh và hấp dẫn. Điều này giúp thế giới bóng đá trở nên thú vị hơn nhiều.
- Hậu trường: Bongdaplus cung cấp tin tức về cuộc sống cá nhân của các cầu thủ, thường là những thông tin nổi bật, scandal và sự kiện đáng chú ý.
- Showbiz: Một chuyên mục mở rộng đăng tin tức liên quan đến các ngôi sao giải trí, ca nhạc, người mẫu và các sự kiện trong làng giải trí.
Bongdaplus có những ưu điểm nổi bật nào?
Ngoài việc có sở hữu đa dạng chuyên mục, bong da plus được đánh giá cao bởi người dùng nhờ vào nhiều điểm mạnh khác nhau. Các khía cạnh này ngày càng được cải tiến với công nghệ hiện đại và chuyên nghiệp, tạo ra trải nghiệm tốt nhất cho người sử dụng.
Giao diện thông minh
Bongdaplus đã tối giản hóa giao diện của mình bằng cách chọn tông màu trắng làm chủ đạo. Đây là một sự lựa chọn màu sắc vô cùng phù hợp cho trang web chuyên đăng tải hàng trăm bài viết liên quan đến bóng đá. Việc sử dụng màu trắng giúp tránh tình trạng quá màu sắc, giúp người đọc không cảm thấy mỏi mắt khi duyệt qua các bài viết. Mặc dù giao diện đơn giản, nhưng trang web Bongdaplus vẫn dễ nhận diện nhờ vào logo màu đỏ kinh điển.
Mỗi ngày, chúng tôi cập nhật hàng trăm bài viết trên trang web, nhưng giao diện của chúng tôi được thiết kế một cách thông minh để đảm bảo tính người sử dụng. Các bài viết được tổ chức rõ ràng vào các chuyên mục khác nhau, và những bài viết nổi bật cũng như mới nhất sẽ xuất hiện đầu tiên. Với câu từ ngắn gọn, đơn giản và dễ hiểu, chúng tôi đảm bảo rằng người đọc có thể dễ dàng nắm bắt thông tin.
Để tăng tính nhận biết, trên trang chính, mỗi tin tức được trình bày với hình ảnh minh hoạ có kích thước nhỏ. Ví dụ, nếu đó là tin liên quan đến một trận đấu, bạn sẽ thấy hình ảnh của hai đội bóng cùng với một tiêu đề ngắn gọn. Các hình ảnh thu nhỏ này không chỉ giúp tạo điểm nhấn mà còn làm cho giao diện của Bongdaplus trở nên hấp dẫn hơn đối với người đọc.
Thông tin chính xác
Tất cả các thông tin xuất bản trên Tạp chí Bóng đá Điện tử này đều được đảm bảo chính xác 100%, nguồn gốc từ các bài báo quốc tế và các cuộc phỏng vấn trực tiếp. Chúng tôi không sử dụng chiêu trò giật tit để tăng lượt xem hoặc viết sai thông tin để thúc đẩy tương tác. Đội ngũ nhân viên của chúng tôi luôn làm việc với tâm lý trách nhiệm, không gây ảnh hưởng đến uy tín của các đối tượng được đề cập.
Đối với các bài viết nhận định về bóng đá và dự đoán kèo, mặc dù không thể đảm bảo chính xác đến 100%, chúng tôi cam kết mức độ chính xác ít nhất là 80%. Bongdaplus không hợp tác với bất kỳ tổ chức nào để đăng tải thông tin không chính xác nhằm dẫn dắt người đọc. Chúng tôi đảm bảo rằng mọi bài viết đều xuất phát từ quá trình thống kê và phân tích của đội ngũ chuyên gia của chúng tôi.
Chuyên gia hàng đầu
Để có được thông tin chất lượng như vậy, không thể không nhắc đến sự đóng góp quan trọng của đội ngũ chuyên gia hàng đầu. Các chuyên gia soi kèo và nhận định bóng đá trong đội ngũ của chúng tôi đều tích lũy được nhiều năm kinh nghiệm, có sự am hiểu sâu sắc về đa dạng các loại kèo. Do đó, nếu bạn là người mới bắt đầu và muốn tham gia cá độ bóng đá, hãy tham khảo ngay các bài viết của họ.
Hơn nữa, mọi thông tin bóng đá trước khi được đăng tải đều trải qua quá trình kiểm duyệt chặt chẽ do đội ngũ biên tập viên uy tín thực hiện. Các bài viết trong mục “Lăng kính bóng đá” trên Bongdaplus được phụ trách bởi những bình luận viên chuyên nghiệp, mang đến cái nhìn độc đáo và có cá tính riêng. Đội ngũ chuyên gia tài năng đông đảo đã giúp kênh chúng tôi đạt được danh tiếng là nguồn thông tin hàng đầu hiện nay.
Website ổn định
Vì là một tạp chí điện tử, trang web Bongdaplus đặt sự quan tâm lớn vào vấn đề đường truyền internet. Hệ thống của chúng tôi sẽ trải qua các công đoạn bảo trì định kỳ để đảm bảo tốc độ tải nhanh, hình ảnh load mượt mà và tiết kiệm dữ liệu internet. Lịch trình bảo trì sẽ được thông báo trước, giúp người dùng có thông tin chuẩn bị. Điều này giúp giảm thiểu khả năng xảy ra tình trạng giật lag khi truy cập dữ liệu tại đây, đảm bảo trải nghiệm trực tuyến suôn sẻ hơn cho mọi người.

Bongdaplus là tổ chức truyền thông chính thức của Liên đoàn bóng đá Việt Nam, đảm bảo sự uy tín cao, hoạt động theo quy định pháp luật và nhận được sự công nhận từ cơ quan chức năng. Trang web của chúng tôi đã duy trì ổn định từ năm 2010 đến nay mà không bao giờ gặp sự cố, đồng nghĩa với việc chỉ có một đường liên kết duy nhất tồn tại và vẫn hoạt động liên tục. Điều này có nghĩa là khi bạn lưu trữ đường liên kết này một lần, bạn có thể sử dụng nó mãi mãi mà không phải lo lắng về bất kỳ sự gián đoạn nào.
Bảo mật an toàn
Cơ quan ngôn luận của Liên đoàn bóng đá Việt Nam, Bongdaplus, đã được thiết lập với mức độ bảo mật cực kỳ cao, mang lại sự an tâm cho người dùng khi truy cập. Không yêu cầu việc đăng ký tài khoản giúp anh em tránh việc phải cung cấp thông tin cá nhân cho trang web để sử dụng các dịch vụ. Điều này giúp giảm bớt lo lắng về việc thông tin cá nhân có thể bị lộ ra bên ngoài.
Ngoài ra, lịch sử truy cập và đọc các bài viết chỉ được hệ thống lưu giữ trong một khoảng thời gian nhất định trước khi bị xoá vĩnh viễn. Hệ thống bảo mật của chúng tôi sử dụng công nghệ hàng đầu hiện nay để đảm bảo mức độ an toàn cao. Các bài viết được đăng không chứa các liên kết độc hại, đảm bảo rằng thiết bị của người dùng không bị nhiễm virus.
Hoàn toàn miễn phí
Bongdaplus cam kết người dùng sẽ không phải chi trả bất kỳ chi phí nào trong quá trình cập nhật thông tin. Kênh này hoạt động phi lợi nhuận, các chi phí sẽ được Liên đoàn bóng đá chịu trách nhiệm và một số tổ chức tài trợ. Mục tiêu chính của kênh là mang đến cho người hâm mộ Việt Nam cái nhìn đa chiều nhất về thế giới bóng đá.
Vì Bongdaplus hoạt động miễn phí, người dùng không cần lo lắng về vấn đề nạp tiền trả phí như một số trang web khác. Đồng thời, nếu có bất kỳ yêu cầu thanh toán nào đối với người dùng, đó có thể là một kịch bản lừa đảo và người dùng cần phải cảnh báo. Mong anh em tránh xa những tổ chức có dấu hiệu gian lận này.
Không chứa quảng cáo
Khi truy cập vào trang web của Bongdaplus, người dùng sẽ không gặp bất kỳ quảng cáo nào làm ảnh hưởng đến trải nghiệm cá nhân. Ngay cả những banner quảng cáo nhỏ nhất cũng không xuất hiện. Bởi vì chi phí hoạt động được đảm bảo bởi Liên đoàn bóng đá, kênh không cần phải dựa vào quảng cáo để có nguồn thu nhập.
Việc không có quảng cáo giúp người dùng không cảm thấy bị quấy rối hoặc không thoải mái. Nội dung bài viết trở nên rõ ràng hơn, với chữ in to và sắc nét, được bố trí một cách khoa học. So với các trang có quảng cáo, rõ ràng rằng các bài viết trên Bongdaplus sẽ không bị ảnh hưởng một cách rõ ràng như vậy.
Phần bình luận chuyên nghiệp
Tại Bongdaplus, bạn không chỉ được cập nhật tin tức miễn phí mà còn có thể thoải mái thể hiện quan điểm và ý kiến của mình trong phần bình luận dưới mỗi bài đăng. Phần bình luận này tương tự như trên các trang mạng xã hội như Facebook, Zalo, Twitter…

Lưu ý rằng trong quá trình bình luận, bạn vui lòng thể hiện thái độ lịch sự và tránh sử dụng các từ ngữ tục tĩu hoặc phản cảm. Đặc biệt, không chèn các đường link không liên quan vào phần bình luận để đảm bảo môi trường an toàn cho các người dùng khác. Nếu hệ thống Bongdaplus phát hiện vi phạm, tài khoản của bạn sẽ bị cấm ngay lập tức nhằm bảo vệ cộng đồng người chơi.
Khi viết bình luận, bạn có thể lựa chọn giữ thông tin cá nhân hoặc sử dụng chế độ ẩn danh. Nếu bạn cảm thấy thoải mái hơn khi giữ ẩn danh, hệ thống cũng hỗ trợ lựa chọn này. Sự linh hoạt này đã nhận được sự đánh giá tích cực từ đông đảo người chơi.
Bongdaplus cập nhật tin tức liên quan đến những giải đấu nào?

Hiện tại báo bóng đá plus đang cung cấp thông tin liên quan đến cả trăm giải đấu bóng đá chuyên nghiệp khác nhau trên hành tinh này. Do đó kiến thức của bạn sẽ được phong phú hơn, bạn sẽ biết đến những danh thủ tài năng không phân biệt quốc tịch. Cụ thể là:
- Bóng đá Việt Nam: Hạng nhất, V League, Cúp quốc gia, bóng đá nữ…
- Bóng đá Anh: Ngoại hạng Anh, FA Cup, League Cup…
- Bóng đá Tây Ban Nha: Cúp Nhà Vua, La Liga…
- Bóng đá Italia: Coppa Italia, Serie A…
- Bóng đá Đức: Cúp QG Đức, Bundesliga…
- Bóng đá Pháp: Ligue 1, Cúp QG Pháp, Cúp Liên đoàn Pháp…
- Một số giải đấu cấp câu lạc bộ: Champions League, Europa League, Club World Cup, Europa Conference League
- Một số giải đấu cấp đội tuyển: World Cup nam – nữ, EURO, Nations League, Copa America, CAN, Olympic…
- Một số giải đấu cấp khu vực: Asian Cup, Asian Games, AFF Cup, SEA Games…
Với vô vàn các giải đấu như trên đảm bảo kho thông tin của kênh bóng đá plus cực kỳ khổng lồ. Với số lượng hàng trăm giải đấu như vậy, cho dù giải đấu nào bạn đang quan tâm cũng đều được cập nhật nhanh chóng. Không những thế trong tương lai kênh sẽ liên tục theo sát nhiều giải đấu khác như các giải đấu hạng 2…
Hướng dẫn cập nhật tin tức tại Bongdaplus
Bongdaplus không chỉ là một trang web cung cấp thông tin bóng đá mà còn là nơi tích hợp nhiều tính năng và chuyên mục hấp dẫn. Tại đây, bạn không chỉ có cơ hội xem các bài viết nhận định về bóng đá và tin tức miễn phí, mà còn có thể chia sẻ thông tin này với các nền tảng khác. Dưới đây là hướng dẫn sử dụng các dịch vụ tại Bongdaplus:
- Đọc tin tức, bài viết nhận định, bài viết soi kèo, lịch thi đấu, bảng xếp hạng: Bạn chỉ cần nhấn vào chuyên mục mong muốn, sau đó chọn bài viết bạn quan tâm để hiển thị nội dung.
- Chia sẻ thông tin: Dưới mỗi bài viết, bạn sẽ thấy nút “like” và “share”. Nhấn nút “share” và lựa chọn nền tảng mà bạn muốn chia sẻ thông tin. Hoặc bạn có thể sao chép đường link bài viết Bongdaplus để gửi cho bạn bè và người thân.
- Bình luận: Nếu bạn muốn chia sẻ ý kiến của mình, đơn giản chỉ cần lướt xuống cuối bài viết và bấm vào mục “Ý kiến của bạn”. Nhập ý kiến và nhấn “Bình luận”.
Bằng cách này, việc sử dụng các dịch vụ tại Bongdaplus trở nên đơn giản và không tốn nhiều thời gian. Đặc biệt, tính năng bình luận giúp bạn dễ dàng giao lưu và mở rộng kiến thức thông qua trao đổi với cộng đồng người hâm mộ.
FAQ – Tổng hợp câu hỏi thường gặp đối với Bongdaplus

Với 13 năm kinh nghiệm, tạp chí bóng đá điện tử của chúng tôi đã tiếp nhận một loạt câu hỏi và thắc mắc đa dạng từ độc giả. Để hỗ trợ bạn hiểu rõ hơn, chúng tôi cam kết giải đáp những thắc mắc này. Khi bạn đối mặt với tình huống tương tự, hãy tự tin tìm kiếm và giải quyết nó.
Có cần đăng ký tài khoản tại Bongdaplus không?
Trang web bongdaplus, nơi cung cấp dịch vụ xem bóng đá trực tuyến, không đòi hỏi người dùng phải đăng ký tài khoản cá nhân. Điều này giúp việc sử dụng thông tin trở nên đơn giản và thuận lợi, mà không cần lo lắng về vấn đề bảo mật cá nhân.
Tuy nhiên, trang web bd plus vẫn cung cấp chức năng đăng nhập tài khoản cho người dùng có sự lựa chọn. Điểm độc đáo giữa hai tùy chọn này là khi đăng nhập, các bình luận của người dùng sẽ hiển thị tên của họ. Ngược lại, nếu không đăng nhập, tên sẽ được ẩn đi. Việc đăng nhập với tên đảm bảo rằng người dùng có thể tương tác một cách tự tin hơn khi tham gia giao lưu với cộng đồng.
Bongdaplus có cập nhật tin tức về các môn thể thao khác không?
Tạp chí điện tử bongdaplus chuyên sâu trong việc cung cấp thông tin về bóng đá và nhiều lĩnh vực thể thao khác như esport, tennis, bóng rổ, đua xe. Mặc dù không chuyên sâu nhưng dữ liệu vẫn rất đồ sộ.
Ngoài việc cập nhật tin tức thể thao, Bongdaplus còn mang đến nhiều chuyên mục đa dạng khác. Đặc biệt, kênh cập nhật thông tin về lĩnh vực công nghệ (điện thoại, máy tính bảng, thiết bị số,…), xe cộ, bất động sản. Đồng thời, bạn có thể tìm thấy thông tin về thị trường như giá vàng, tỷ giá, giá xăng dầu, thị trường chứng khoán.
Với sự đa dạng này, việc truy cập vào kênh sẽ mang lại cho bạn không chỉ những thông tin hữu ích về thể thao mà còn nhiều kiến thức bổ ích từ các lĩnh vực khác.
Bongdaplus có hoạt động ở các quốc gia khác không?
Vì kênh Bongdaplus là một tạp chí bóng đá điện tử thuộc sự quản lý của Liên đoàn Bóng đá Việt Nam, do đó, hiện tại kênh chỉ phục vụ khán giả trong lãnh thổ Việt Nam. Kênh chỉ hỗ trợ một ngôn ngữ duy nhất là tiếng Việt. Tuy nhiên, nếu bạn đang ở các quốc gia khác, bạn vẫn có thể truy cập trang web bằng cách thay đổi địa chỉ IP của mình thành Việt Nam.
Có thể truy cập Bongdaplus trên điện thoại không?
Hiện tại, kênh chưa hỗ trợ ứng dụng, do đó người dùng không thể tải ứng dụng để xem tin tức bóng đá. Tuy nhiên, bạn vẫn có thể truy cập trang web qua trình duyệt trên điện thoại để đọc tin tức. Các thao tác sử dụng thông tin hoàn toàn giống như trên máy tính.
Website Bongdaplus có cập nhật các video không?
Kênh Bongda Plus không chỉ cung cấp thông tin cho người dùng qua các bài viết được đăng tải, mà còn hỗ trợ thông qua nền tảng video để đáp ứng nhu cầu đa dạng của khán giả. Các video bao gồm:
- Video Highlights: Tập trung vào những điểm nổi bật và các diễn biến quan trọng của trận đấu. Các video này sẽ được đăng tải ngay sau khi trận đấu diễn ra, có thời lượng khoảng 10 phút mỗi trận.
- Video Tin Tức Hàng Ngày: Bongdaplus sẽ đăng tải video này mỗi ngày để cung cấp những tin tức nóng hổi nhất về bóng đá.
- Video Soi Kèo Bóng Đá: Những video này hứa hẹn mang đến những lựa chọn đặt cược chính xác nhất, làm hài lòng những người yêu thích cờ bạc thể thao.
- Video Nhận Định Bóng Đá: Cung cấp góc nhìn toàn diện nhất về trận đấu sắp tới, giúp khán giả có cái nhìn tổng quan và hiểu rõ hơn về cảnh đấu sắp diễn ra.
Kết luận
Bongda Plus đã trở thành lựa chọn hàng đầu của cộng đồng người hâm mộ bóng đá Việt Nam, được đánh giá cao với tư cách là kênh bóng đá trực tuyến uy tín nhất. Do đó, số lượng người truy cập mới không ngừng tăng lên mỗi ngày. Nếu bạn cũng chia sẻ niềm đam mê với hàng triệu người hâm mộ trên khắp thế giới, hãy truy cập ngay vào trang web bongdaplus này.

 Danh sách giải đấu
Danh sách giải đấu

